We present a rather unusual case of recurrent stone disease and on investigation found to have hyperparathyroidism (Sr. PTH 219.3 pg/ml, Sr Calcium 12.4 mg/dl, Alkaline phosphatase 87, Sr Creatinine 0.87). On 99mTc Sestamibi parathyroid hybrid SPECT CT imaging three metabolically active parathyroid adenomas were identified, which was reconfirmed on CT Neck W & W/O contrast pre-operatively. Subsequently patient underwent three gland parathyroidectomies & histopathology showed three gland parathyroid hyperplasia.
Parathyroid adenoma is the most common cause of primary hyperparathyroidism (pHPT). Adenomas usually involve only a single gland, and the remaining glands are normal or suppressed. Occasionally, two or three parathyroid adenomas are found in a single patient; however, the occurrence of three true adenomas is exceedingly unusual. When more than one adenoma is encountered, the possibility of parathyroid hyperplasia should be considered. The significant incidence of multiple adenomas with histologic similarities to hyperplasia has raised the possibility that adenoma is a continuation of the hyperplasia state.
Hyperparathyroidism can be caused by both parathyroid adenomas and parathyroid hyperplasia. The result of having parathyroid adenoma or hyperplasia is the same: hyperparathyroidism symptoms and consequences. But the way a parathyroid adenoma develops is very different then hyperplasia, and the treatment is also a different surgery
A parathyroid adenoma is a benign tumor that develops inside a parathyroid gland and continually grows. As it grows it produces PTH that causes calcium’s to get higher thus leading to hyperparathyroidism. The other three remaining parathyroid glands are normal. Parathyroid hyperplasia is a condition where all parathyroid cells in all parathyroid glands are abnormal, causing all the glands to grow and produce PTH and again causing hyperparathyroidism. The extra PTH production happens in all 4 glands, and there are no remaining normal parathyroid glands.
Parathyroid glands have each million of cell in them. All these parathyroid cells have calcium sensor (Calcium Sensing Receptor or CaSR) that has a genetically predetermined calcium setting. This means all the parathyroid cells in all 4 glands normally try to keep the blood calcium level the same number the entire life of a human being. If one of these cells in one parathyroid gland gets exposed to a toxin that causes a mutation in it that changes the setting for calcium to a higher number, then that cell (not realizing it is making a mistake) will do everything it can to bring the blood calcium level to that higher number.
As an example, if the person’s normal calcium setting is 9.0 mg/dL, and one cell develops a mutation in the calcium sensing mechanism (like a change in the thermostat setting), making the mutated parathyroid cell want a higher calcium level. The mutated parathyroid adenoma cell that is trying to make the blood calcium level be higher, works hard to achieve this. In the process it keeps duplicating itself and getting bigger and bigger. Parathyroid adenomas start very small but in time grow to be large (almost one inch long). They only cause problems because they produce hormone not because they get large enough to push on the surrounding tissue; they don’t directly cause neck pain or breathing issues. They don’t’ have any nerves growing into them, so they are not felt.
Rarely, parathyroid adenomas may appear in more than one gland at the same time. They each may produce different amounts of PTH causing the elevation in calcium. Adenomas in two glands are uncommon (10%), and adenomas in 3 glands (although they do occur), are exceedingly rare.
Parathyroid 4 gland hyperplasia develops because all the cells in all 4 parathyroid glands are abnormal. Each parathyroid gland has roughly 5 million cells within it. These cells have genetic mutations in them that cause them to continually grow (Figure 3). At the same time, they seem to have a tolerance for elevation in calcium. The rate of growth may be different for each these glands thus most often at the time of surgery one finds that each gland may be a different size. Some may have such a slow growth rate that they may appear normal. As these glands grow, they produce more PTH, slowly elevating the calcium level in the blood stream. On occasion a parathyroid adenoma may develop in one of these glands.
46 years old geneleman with hisroty of recurrent renal stone dissease .on work up found to have hyperparathyroidism
Sr. PTH 219.3 pg /mL (15-68), Sr calcium 12.4 mg/dl (8.8-10.6), Sr. TSH IU/ml (0.45- 4.7), Sr phosphorous 2.9 mg/dl (2.3-4.3), Alkaline phosphatase 87 U/l (40-129), Sr creatinine 0.87)
USG Neck- Mild diffuse enlargement of thyroid with two heterogenous nodules are seen in right lobe (8.9*6.9 and 7.6*3.6 mm) and small hypoechoic nodule (3.7*2.4 mm) in left lobe – MNG
It shows focal areas of abnormal MIBI tracer accumulation in:
a) Inferior to the right lobe of thyroid gland posteriorly (approximately 1.8*1.2. cms in size & appreciated in Static & Hybrid SPECT-CT IMAGES) b) Upper portion of the left lobe posteriorly (approximately 1.6*1.1 cms in size & appreciated in Static and Hybrid SPECT-CT IMAGES) c) Mid portion of left lobe posteriorly (approximately 1.3*1.0 cms in size & appreciated in Static & Hybrid SPECT CT images) on initial images.
(Figures 1,2,3,4,5, 9,10,11, & 12)
On delayed images there is persistent tracer retention of varying tracer intensity is seen in same areas (a,b,c) (Figures 1,6,7,8,9,10,11 & 12)
While rest of the gland shows good MIBI tracer uptakes on initial images and adequate washout pattern on delayed images.
The right lobe measures 4.7*1.7 cms in size and left lobe 4.1*1.7 cms in size approximately and shows mildly patchy tracer uptakes with no obvious hot/cold areas.
MULTIPLE METABOLICALLY ACTIVE PARATHYROID ADENOMAS A TO C. Advised- HRCT with contrast preoperatively

Figure 1: Static 99mTc Sestamibi parathyroid (initial and delayed) & 99mTc thyroid images
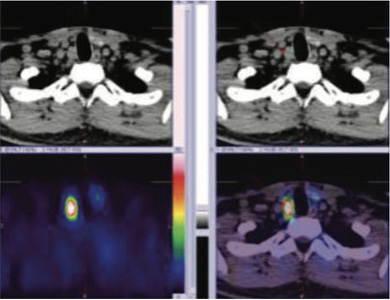
Figure 2: 99mTc MIBI initial hybrid SPECT CT images showing parathyroid adenoma ( PA1) in inferior to the lower portion of right lobe posteriorly
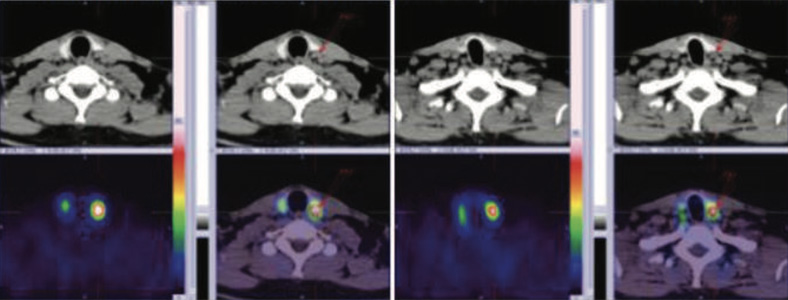
Figure 3 & 4: 99mTc MIBI initial hybrid SPECT CT images showing parathyroid adenoma ( PA2) in upper portion of left lobe r portion posteriorly and PA3 in mid posterior posrtion of left lobe of thyroid gland.as shown with arrows.
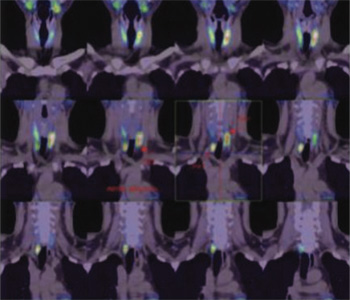
Figure 5: 99mTc MIBI initial hybrid SPECT CT images showing parathyroid adenomas ( PA1) (PA2) & (PA3) as shown with arrows.
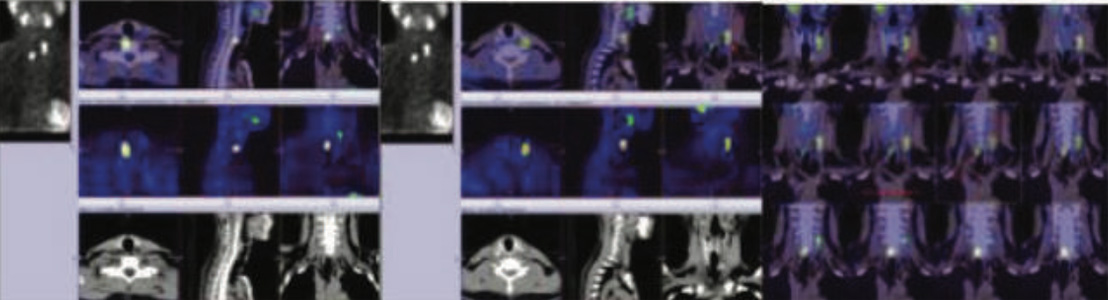
Figure 6,7,8: 99mTc MIBI DELAYED hybrid SPECT CT images showing parathyroid adenomas ( PA1) (PA2) & (PA3) as shown with arrows
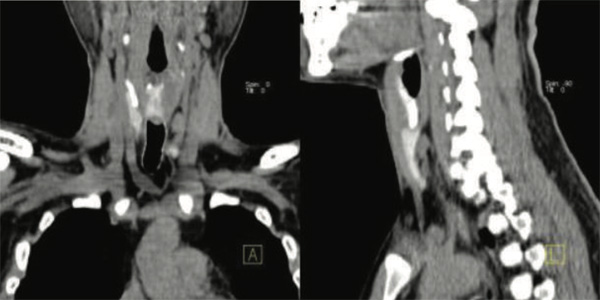
Figure 9 & 10: Underlying CT images showing showing parathyroid adenomas ( PA1)
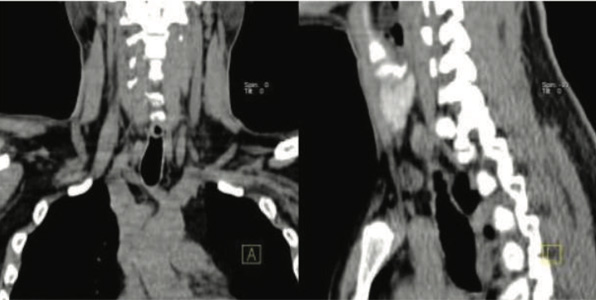
Figure 11 & 12: Underlying CT images showing showing parathyroid adenomas ( PA2 & PA3)
Well circumscribed 21*12*9 mm sized, moderate, and inhomogeneous enhancing, ovoid soft tissue attenuation solid lesion in the right paratracheal region, posteroinferior to the lower pole of the right lobe. No internal calcification/necrosis. This lesion is fed by a branch of right inferior thyroid artery. The distance between the margin of the thyroid gland & this lesion is 5 mm with fat interposed in between them.
Well circumscribed 18*11*6 mm sized, moderate, and inhomogeneous enhancing, ovoid soft tissue attenuation solid lesion posterior to upper of pole of the left lobe of thyroid. No internal calcification/necrosis. This lesion is fed
by a branch of left superior thyroid artery. The distance between the margin of the thyroid gland & this lesion is 1 mm with fat interposed in between them.
Well circumscribed 15*6*4 mm sized, moderate, and inhomogeneous enhancing, ovoid soft tissue attenuation solid lesion posterior to mid pole of the left lobe of thyroid. No internal calcification/necrosis. This lesion is fed by a branch of left superior thyroid artery. The distance between the margin of the thyroid gland & this lesion is 1 mm with fat interposed in between them.
Three, well circumscribed, moderate & inhomogeneous enhancing ovoid shaped soft tissue attenuation solid lesions as described above. In view of High Sr. PTH, Sr calcium and 99mTc Sestamibi findings, it represents multiple parathyroid adenomas.
Subsequently patient underwent three gland parathyroidectomies & histopathology showed three gland parathyroid hyperplasia.
Primary hyperparathyroidism (PHPT) is a common endocrine disorder and Preoperative biochemical and imaging study results reliably distinguished single-gland vs multi-gland parathyroid disease in primary hyperparathyroidism.
Patients with PHPT have a single parathyroid adenoma (80%-87% of patients), multiple adenomas (2%-5% of patients), asymmetric 4-gland hyperplasia (10%-15% of patients), or carcinoma (<1% of patients) that secretes an inappropriately high parathyroid hormone (PTH) level relative to the serum calcium level. Parathyroidectomy is the only curative treatment for PHPT that resolves metabolic complications and improves symptoms and quality of life.
Both parathyroid adenoma and hyperplasia can present with elevations of calcium & PTH, they can also present as normo-calcemic HPT or normo-hormonal HPT. So based on lab tests alone one can’t reliably distinguish between an adenoma or hyperplasia. Having said that when PTH levels are above 150 pg/mL the chance of hyperplasia is around 5%, while with PTH levels lower than 100 pg/mL the chance of hyperplasia goes up by 3-4 folds. But even at low PTH numbers the chance of parathyroid adenoma is significantly higher (75%) then hyperplasia.
When hyperparathyroidism patients have two or more localization studies (ultrasound, Sestamibi hybrid SPECT-CT, or CT scan w & w/o contrast scan) that are negative, or not able to find an enlarged over-active gland, then the odds of that person having hyperplasia is also higher. This makes sense because if all 4 glands are only slightly larger than normal, but all are producing extra hormone (PTH), then each parathyroid gland may not need to be so large to have a deep impact on the person. Because of this slight enlargement they may not be visible on scans.
Although in most cases of primary hyperparathyroidism due to the development of parathyroid hyperplasia is likely a slower more gradual process, it is hard to be able to figure that out without having calcium, PTH & vitamin D labs for many years. Unfortunately, most people don’t have these blood tests done on a routine basis.
A false-negative localizing result was defined as when 1 or more enlarged parathyroid glands were not identified. No true-negative results could occur because all of the patients had biochemical evidence of PHPT consisting of elevated or inappropriately high total serum calcium levels and elevated or inappropriately high intact PTH levels. Concordant localizing study findings were defined as showing 1 enlarged parathyroid gland on the same side of the neck.