The prevalence of primary hyperparathyroidism with proven diabetes mellitus is around 0.1% and hyperparathyroidism is associated with abnormalities in glucose tolerance and insulin secretion.
In patients with hyperparathyroidism, the coexistence of diabetes mellitus might be a further indication for parathyroidectomy. Physicians should be alerted to the possible change in diabetic regimen and the risk of hypoglycemia in patients with diabetes after parathyroidectomy.
Disturbances of glucose metabolism with hyperinsulinism and peripheral insulin resistance are frequently observed in patients with hyperparathyroidism. The mechanism of how hyperparathyroidism affects glucose metabolism is not known. Hypercalcemia, hypophosphatemia and the parathyroid hormone itself seem to be involved. However, parathyroidectomy exerted rather variable effects on glucose metabolism: In patients with fully developed diabetes mellitus both, a complete normalization of glucose tolerance as well as no change in the metabolic situation have been observed
We report two cases of diabetes mellitus in a middle-aged male who subsequently developed primary hyperparathyroidism and one of them underwent parathyroidectomy
49 years old gentleman with long-standing history of Type 2 Diabetes with diabetic neuropathy. Complaining of uneasy feeling in both the legs (difficult to explain the symptoms), paresthesia of skin & insomnia since last one month and found to have uncontrolled diabetes.
On routine Biochemistry work up found to have hyper-parathyroidism
Biochemistry
PTH 116.2 pg /mL (15.0-68.3), Sr calcium 2.8 mmol/L (2.18-2.60), Sr phosphorus 1.0 mmol/L (0.78-1.65), Sr Alkaline Phosphatase 100 IU/L (46-116), Vitamin B12 640 pmol/L (156-672) TSH 0.609 mIU/ml (0.55-4.78).
Ref for 99mTc SESTAMIBI PARATHYROID SCINTIGRAPHY
99mTc-MIBI PARATHYROID IMAGES (Dual isotope technique)
EARLY AND DELAYED MIBI IMAGES OF NECK AND CHEST It shows focal area of increased MIBI tracer uptakes (approximately 7.0*3.3 mm in size) seen infero-posterior portion of the left lobe of thyroid gland (Appreciated in SPECT-CT fused images) and persistent tracer retention in the same region on delayed washout images.
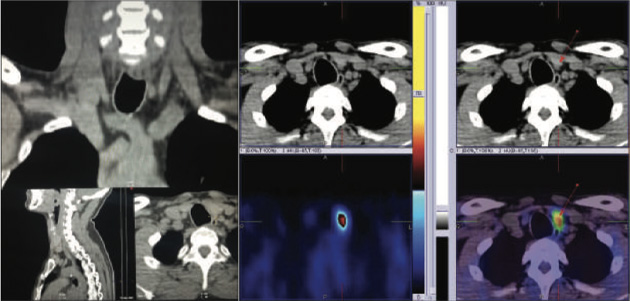
Figure 1- CT images of neck & 2- axial hybrid SPECT CT fused images showing parathyroid adenoma in inferio-posterior portion of the left lobe of thyroid gland (as shown with arrows).
99mtc Mibi Parathyroid Hybrid Spect Ct Images Show Small Sized Focal Metabolically Active Parathyroid Adenoma (Approximately 7.0*3.3 Mm In Size) Seen Inferio-posterior Portion Of The Left Lobe Of Thyroid Gland (Figure 1 To 4 As Shown With Arrow).
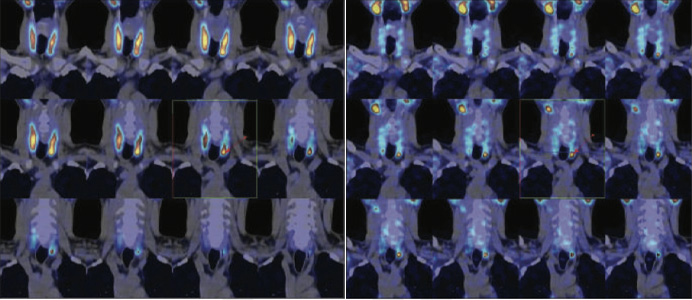
Figure 3-Early & 4-Delayed images
99mTcMIBI hybrid SPECT CT fused images showing parathyroid adenoma in inferio-posterior portion of the left lobe of thyroid gland (as shown with arrows).
47 years old gentleman with long-standing history of Type 2 Diabetes. Recently found to have uncontrolled diabetes with no other symptoms.
On routine Biochemistry work up found to have hyper-parathyroidism
Biochemistry
PTH 95 pg /mL (15.0-68.3), Sr calcium 2.7 mmol/L (2.18-2.60), Vitamin B12 120 pmol/L (156-672, TSH 1.74 mIU/ml (0.55-4.78).
Ref for 99mTc SESTAMIBI PARATHYROID SCINTIGRAPHY
99mTc-MIBI PARATHYROID IMAGES (Dual isotope technique) EARLY AND DELAYED MIBI IMAGES OF NECK AND CHEST
It shows small focal area of minimally increased MIBI tracer uptakes at the inferior pole of left lobe of thyroid gland on early images (Better appreciated in SPECT-CT fused images), while on delayed shows marginal tracer retention in the same region (figure 1 to 4).
Rest of the thyroid gland shows mildly patchy and relatively decreased MIBI tracer uptakes in thyroid gland on initial images and adequate washout pattern on delayed images.
Parathyroid mechanism uptake-Mitochondria-rich oxyphil cells presumably account for MIBI uptake in parathyroid lesions. Fewer oxyphil cells, and hence fewer mitochondria, may explain both lower uptake and rapid washout of MIBI from some lesions. Parathyroid adenomas that express either P-glycoprotein or the multidrug resistance related protein MRP are less likely to accumulate MIBI. MIBI scintigraphy is less sensitive for detecting hyperplastic parathyroid glands.

Figure 1 - 99mTcMIBI Static Early And Delayed Images showing minimally active parathyroid adenoma at the inferior pole of the left lobe of thyroid gland.
99mTc MIBI PARATHYROID HYBRID SPECT CT IMAGES SHOW SMALL SIZED MINIMAL METABOLICALLY ACTIVE PARATHYROID ADENOMA AT THE INFERIOR POLE OF THE LEFT LOBE OF THYROID GLAND (figure 1 to 4).
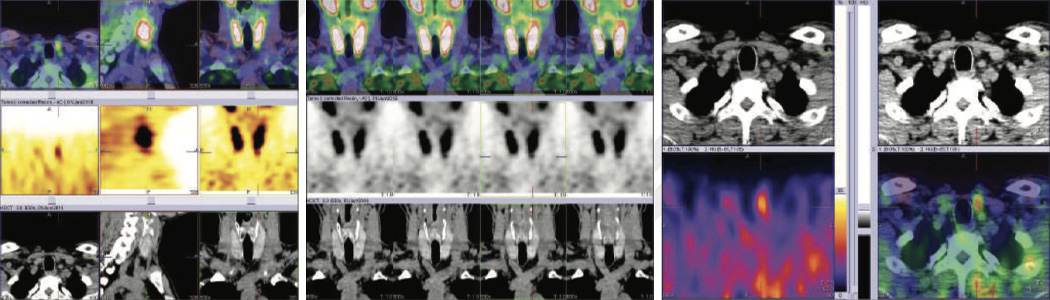
Figure 2,3,4 - 99mTcMIBI Hybrid SPECT CT fused images showing minimally active parathyroid adenoma at the inferior pole of the left lobe of thyroid gland.
An oval lesion with smooth margins located at the inferior pole of the left hemi thyroid. In view of the enhancement characteristics (washout of the contrast material from the arterial to delayed phase, the possibility of a parathyroid adenoma seems more likely than a sub centimeter sized lymph node.
Underwent inferior pole left lobe parathyroid adenoma resection and histopathology shows nodular cellular parathyroid tissue consistent with parathyroid adenoma/nodular hyperplasia.
The prevalence of diabetes mellitus (DM) or glucose intolerance in PHPT and prevalence of primary hyperparathyroidism in diabetic patients are about three-fold higher than their respective expected prevalence’s in the general population.
The response of parathyroid surgery on diabetes is variable: in some patients the diabetic condition improves or resolves. The type of diabetes associated with PHPT is also variable: Type 1 or Type 2.
The clinical and laboratory investigations on the influence of hyperparathyroidism on DM support the benefit of parathyroidectomy in patients with DM. Patients with type 1 and type 2 DM show improvement in glucose control after parathyroidectomy. The presence of DM and hyperparathyroidism is an indication for parathyroidectomy because it results in either stabilization or improved glucose control in 77% of patients. Previous reports have suggested that control of diabetes improves after successful parathyroidectomy for primary hyperparathyroidism