Prostate cancer (PC) is the second most frequent cancer and the sixth leading cause of cancer death in men worldwide.When detected early, prostate cancer has more than a 90 percent cure rate. Because treatment is highly individualized, molecular imaging technologies are dramatically improving the ways in which prostate cancer is diagnosed and treated.
Broadly defined, molecular imaging is the non-invasive detection and measurement of cellular and molecular processes in whole living beings using a variety of modalities including positron emission tomography (PET), single photon emission computed tomography (SPECT), magnetic resonance (MR), computed tomography (CT), ultrasound, fluorescence, or bioluminescence.
Conventional imaging modalities, including bone scintigraphy (bone scan), CT, ultrasound, and MR imaging, are currently used to detect primary PCa and and metastatic disease for staging and risk stratification.
PSMA (Prostate Specific Membrane Antigen) is a membrane glycoprotein which is overexpressed manifold on prostate cancers.
The expression increases with tumor aggressiveness, androgen independence, metastatic disease, and disease recurrence. u
PSMA is an excellent target for radionuclide imaging and therapy of prostate cancer for several reasons.
It is mainly expressed in prostate cancer in all stages of the disease, up-regulated in androgen refractory or
metastatic disease, expressed on the cell surface as an integral membrane protein, not released into the
circulation, and internalized after antibody binding (receptor-mediated endocytosis) u
99mTc PSMA SPECT/CT Imaging identifies tumor cells expressing PSMA antigen with excellent sensitivity &
specificity, thereby detecting lesions remaining unidentified by conventional methods.
SPECT-CT Imaging with 99mTc-PSMA ligand can present lesions suspicious for prostate cancer with excellent contrast and a high detection rate even when the level of prostate specific antigen is low. PSMA expression allows the identification of benign and malignant prostatic epithelium and may be a potentially valuable marker in the treatment of patients with prostate cancer.
99mTc-PSMA SPECT-CT has promising potential for restaging in recurrence/ biochemical failure after definitive treatment of prostate cancer.
99mTc-PSMA SPECT-CT could be used as a marker of patient response to anti-androgen drugs.PMSA studies are able to determine the extent of prostate cancer and whether it has spread to the lymph nodes or other parts of the body.Unlike traditional imaging technologies such as magnetic resonance imaging (MRI) and computed tomography (CT), which are often unable to detect the spread of prostate cancer cells.
Comparison of different imaging modalities for metastatic lesions in PCa patients. Prostate-specific membrane antigen (PSMA) single-photon emission computed tomography (SPECT)/computed tomography (CT) imaging provided a higher detection ratio.
99mTc labeled PSMA
Nil
A patient is injected intravenously with the 99mTc-PSMA (600 to 800 MBq on a average). WHOLE BODY AND SPECT-CT fused images at 5-6 and 20-24 hours respectively (approximate imaging timings takes 30 to 45 minutes). Between 6 and 18 hours P.I. there is best time window for the imaging.
PSMA-SPECT/CT imaging identified more metastatic lesions and provided a higher detection rate than conventional imaging modalities and is helpful in clinical diagnosis and treatment.
46 yrs old gentleman with history of chronically elevated PSA (total ) 10.12 ng/ml (0.00-4.00). MRI prostate (16.3.2018)-Mild symmetrical prostatomegaly, matching with BPH. Prostate biopsy (two times in 2017)- Negative for malignancy.
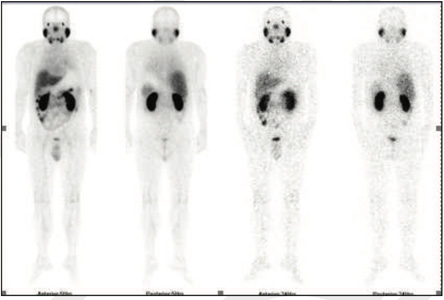
Figure 1: 99mTc-PSMA Whole Body Images
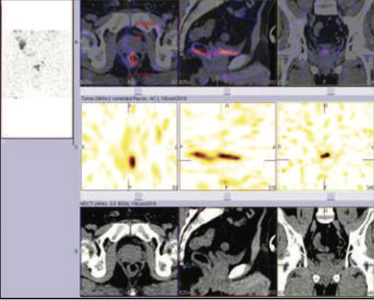
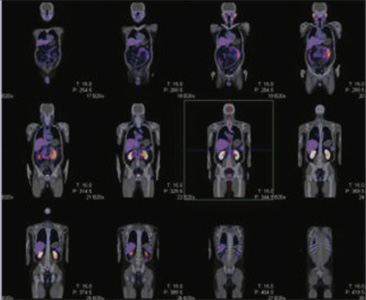
Figure 2&3: 99mTc-PSMA SPECT-CT IMAGES No PSMA expression lesions are seen in prostate gland or elsewhere on whole body images.
87 yrs old gentleman with history of repeated difficulty in urination, dysuria USG- symmetrical prostatomegaly and high residual urine. H/o chronically elevated PSA (total ) 25.55 ng/ml (0.00-4.00). Free PSA 6.07 ng/ml
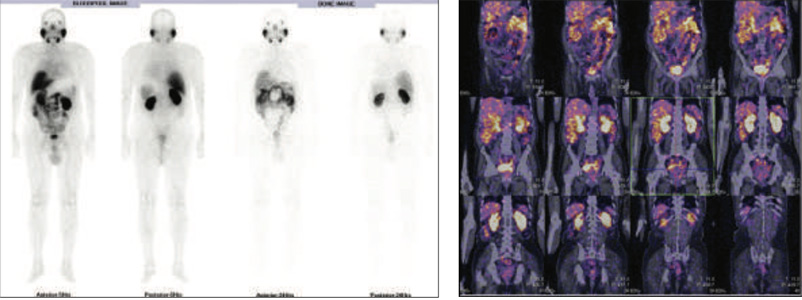
Figure 1 & 2: 99mTc-PSMA Whole Body & SPECT CT fused Images
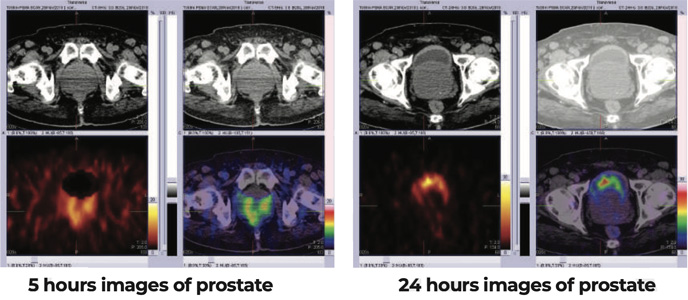
Figure 3 & 4 : 99mTc-PSMA SPECT-CT IMAGES OF PELVIS
72 yrs old gentleman. PSA (total ) 20.22 ng/ml (0.00-4.00),PSA (free) 2.750 ng/ml. MRI prostate (9.10.2017)-Moderate symmetrical prostatomegaly with preferential enlargement of the central/transitional zones showing overall multi-parametric data, matching with BPH, associated with small lesion related to the right perepheral zone of low grade suspicion, for correlation with serum PSA. Prostate biopsy (19.10.2017)- Focal chronic prostatitis and negative for malignancy.
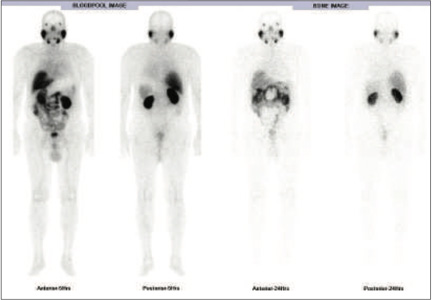
Figure 1 : 99mTc-PSMA Whole Body Images
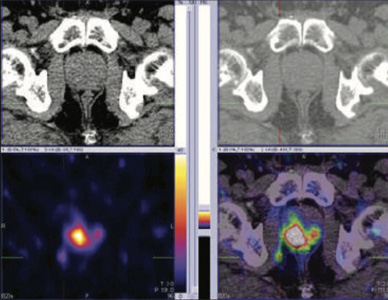
Figure 2: 99mTc- PSMA SPECT CT fused images of pelvis Abnormal PSMA tracer accumulation in a) right peripheral zone (high uptakes), b) left peripheral zone (mild uptakes) and c) right pelvic lymph node. Rest of the whole body images were unremarkable
Prostate biopsy (25.1.2018)-Prostate adenocarcinoma in all six biopsies. Tumor involves 70% of total slide area on the right side and nearly 50% on the left side. No perineural or lympho-vascular invasion noted. Gleason scare 6
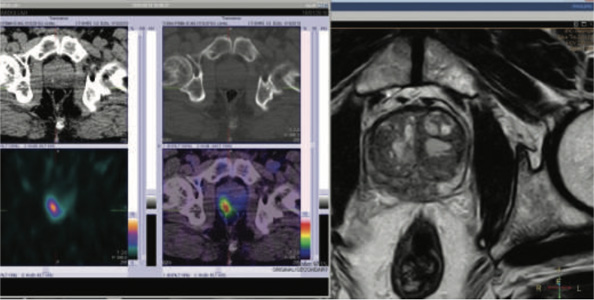
Figure 3 & 4: 99mTc- PSMA SPECT CT & MRI post rebiospsy correlation
66 yrs old gentleman. H/O Radicle prostectomy 4 years ago.
HP (3.3.2011)- A diffuse nodular lesion noticed posteriorly on both right and left side (predominant on right ) made up of adeno-carcinomatous tissue, invading a) directly into normal glandular elements of the prostate b) into peri-neural lymphatics c) into wall of the vascular channels ( tumor did not infiltrate the whole thickness of the capsule).Gleason score = 6
PSA (0.22-6.16)
2025 - 0.987
2016 - 1.173
8.11.2017 - 2.340 (Casodex 50 mgm)
27.12.2017 - 0.454 (on medication)
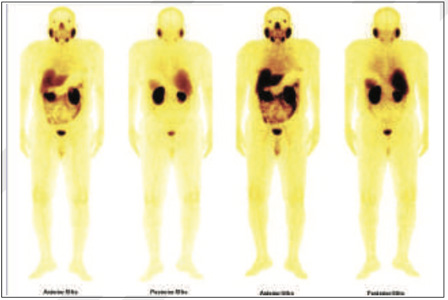
Figure 1: 99mTc-PSMA Whole Body Images
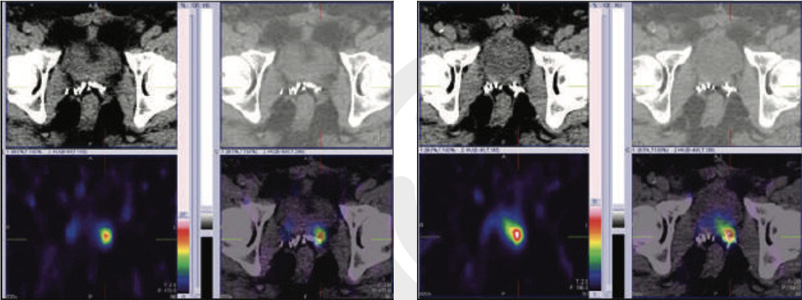
Figure 2 & 3 : 99mTc- PSMA SPECT- CT fused images Abnormal PSMA tracer accumulation in left prostatic bed (Better appreciated in SPECT-CT FUSED images at 5 & 20 hours images).
Rest of the whole body images were unremarkable.
56 yrs gentleman. H/O Abnormal PSA 6.0 ( 5 yrs ago) à Rx with antibiotics.
PSA 4.0-> recent PSA 15.4 but no other obvious symptoms.
MRI prostate (17.1.2018)-Well defined smooth margined abnormal signal intensity lesionInvolving anterior
fibro-muscular stroma & transitional zone near base region and mid part of the prostatic gland from 9 to 1 clock
position. Considering morphology and anatomical location of the lesion, the possibility of benign looking lesion/focal
infection appears likely. However in view of persistent elevated PSA : biopsy examination is recommended.
Prostate biopsy (6.2.2018) HP- primarily a very well differentiated adeno-carcinoma of right side of prostate. No
peri-neural invasion identified. Left side of prostate shows few atypical glands and prostatic intraepithelial neoplasm.
Gleason score-6
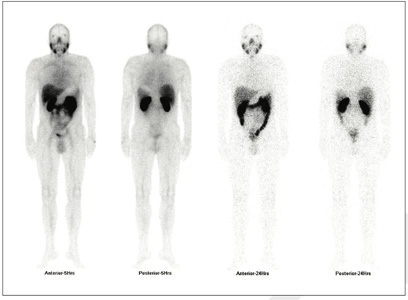
Figure 1 : 99mTc-PSMA Whole Body Images
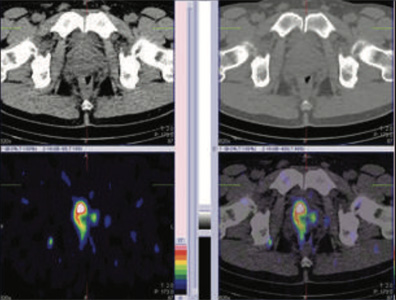
Figure 2 &\ 3: 99mTc- PSMA SPECT- CT fused images of pelvis Focus of cancer in right prostatic bed as well as in left prostatic bed (right >>> left) along with suspiciously in right pelvic lymph node. Rests of the whole body images were unremarkable Case-6 (Extensive metastatic bone disease)
82 yrs gentleman with h/o Prostatectomy 15 yrs ago and known case of metsatstaic prostatic cancer.
FDG F18- PET-CT (30.6.2014)
Intense FDG uptake noted within left facet joint L4 ( SUV max 4.6) with possible expansion of the underlying marrow ? Worrisome. Adv- MRI
PSA (total ) 1492 ng/ml (<4.00) 10.1.2017
PSA TOTAL 2060 ng.ml ( < 4.00) 9.7.2017) and on adelateron Rx 250 mgm TDS
PSA TOTAL 316 ng/ml ( <4.0) 6.1.2018
MDP whole body bone scan (8.6.2017)- Extensive bony metastasis
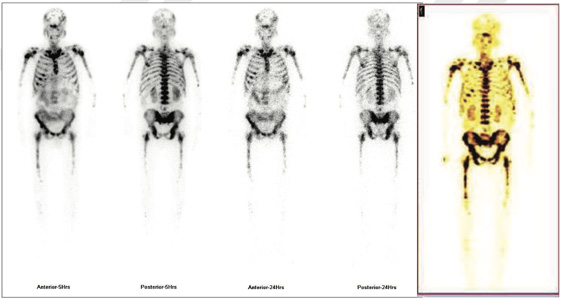
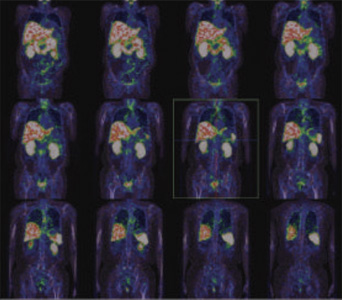
Figure 1 & 2: 99mTc-PSMA Whole Body Images & 3D whole body images

Figure 3 : 99mTc- PSMA SPECT- CT fused images of pelvis
Abnormal PSMA tracer accumulation seen involving most of the skeletal system. No abnormal tracer uptakes in prostatic bed nor in lymph nodes.
Extensive metastatic bone disease. No abnormal focus in prostatic region nor in any lymph nodes.
62 yrs old gnetleman with h/o PSA (total ) 8.02 ng/ml (<4.00) 24.4.2018 and Free PSA 3.76 ng/ml. MRI Pelvis- Heterogeneous low to intermediate signal change is seen in the right 2/3rd of the prostate gland involving the central and peripheral zones suggestive of neoplastic disease. Features are more likely to represents adenocarcinoma of the prostate. Biopsy advised. Bilateral enlarged obturator and left iliac lymph nodes are seen suggestive of nodal metastasis.
Prostate biopsy- Right lobe- Poorly differentiated adenocarcinoma (Gleason score 3+4=7) involving six core biopsies occupying approximately 40% of the tissue with circumscribed peri-neural invasion. Left lobe- Moderately differentiated adenocarcinoma ( Gleason score 3+3=6) involving 4 of the 6 core biopsies occupying approximately 20% of the tissue.TNM- pTx,G3 ( Gleason score 3+4=7).
H/o severe prostatitis post biopsy

Figure 1 & 2: 99mTc-PSMA whole body images & SPECT CT fused images of pelvis
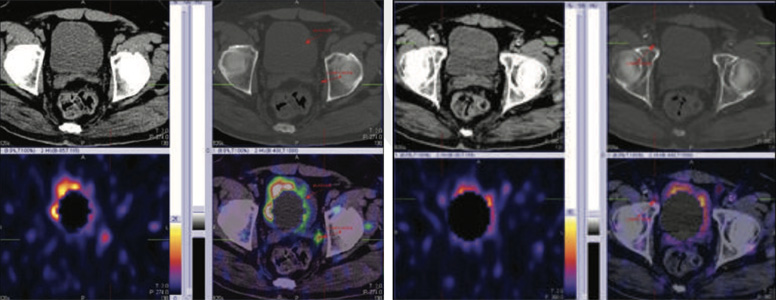
Figure 3 & 4: 99mTc-PSMA SPECT CT fused images of pelvis
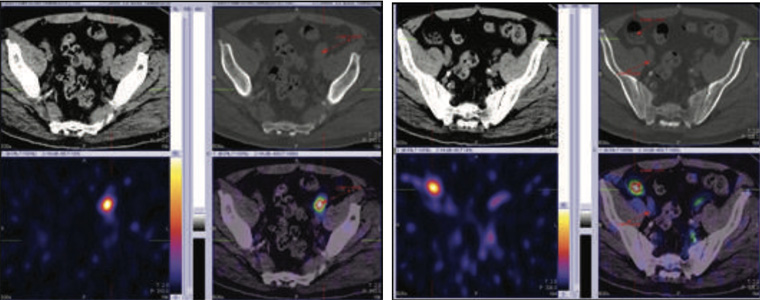
Figure 5 & 6: 99mTc-PSMA SPECT CT fused images of pelvis
99mTc- PSMA whole body images & SPECT- CT fused images of pelvis Fairly large focal area of abnormal PSMA tracer accumulation seen in peripheral zone in midline of the prostatic bed.
In addition to this, there is abnormal PSMA tracer accumulation in obturator lymph node ( moderate uptakes) and external iliac lymph nodes ( high uptakes) on the left side approximately. Lateral vesicle lymph node (minimal uptakes) on right side approximately.
79 yrs old gentleman underwent TURP for BPH in 2016 (h/o urinary retention).
Histopathology- Disclosed fragment of of prostate tissue. Almost all of them are infiltrated by sheets of prostate
adenocarcinoma ( Gleason score to be 7).
Was put on tablet casodex- Two month later patient stopped and lost follow up.
PSA (total ) 55.031 ng/ml (0.21-6.77) 25.7.2016
PSA ( total) 71.690 ng/ml (0.0-4.0) 16.9.2018
USG KUB (16.9.2018) Prostate- is normal in size and heterogeneous echo texture. It measures 3.6*2.78*3.68 cms.
Volume is 17.5 ml. It shows central defect ? Partial resection. No focal lesion or calcification seen.
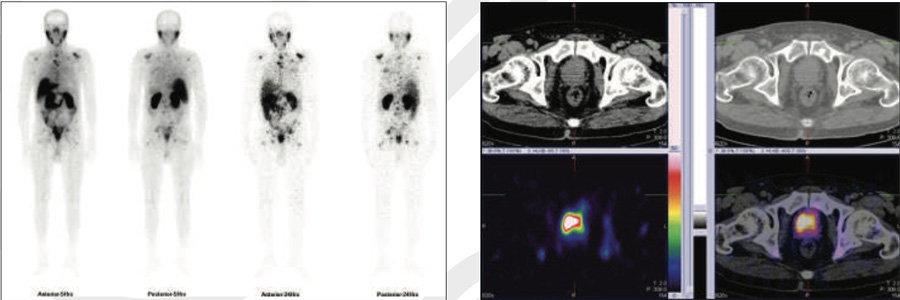
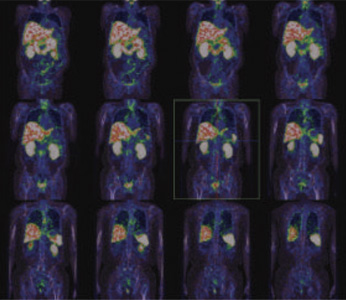
Figure 1 & 2: 99mTc-PSMA whole body images & SPECT CT fused images of the pelvis
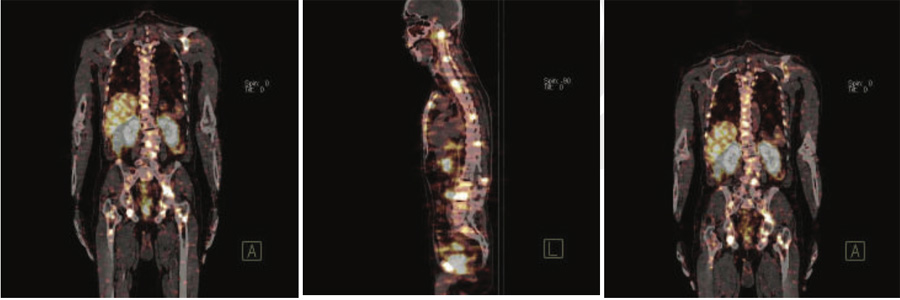
Figure 3,4 & 5: 99mTc-PSMA whole SPECT CT fused images
PSMA avid areas of abnormal tracer uptakes in C1,C5,C7,D1,D5,D6, D7,L1,L5,S1vertebrae.Manubri sternum. Multiple ribs (1st,5th10th and 12th rib-right and 11th rib-left),Both the glenoids ( left>right).Left anterior iliac spine. Both the acetabular regions. Both ischeal bones. Both iliac bones. Both the trochanteric regions. Proximal shaft of right femur. No obvious abnormal PSMA uptakes seen in lymph nodes, Liver, Lung and brain etc. ABNORMALITIES REPRESENTSPROSTATIC CANCER WITH BONY METASTASIS
69 yrs old gentleman with h/o PSA (total ) 57.150 ng/ml (<4.00) 5.9.2018 and Free PSA 2.59 ng/ml.
MRI PROSTATE- Right side –lesion-1 seen in peripheral zone. 1.6 cms in size but contiguous with the lesion involving seminal vesicle with contact to the capsule. shows low intesnsity signal in T2 and ADC images and high signal in DW1 images (score 5). Enhances following contrast media.Lesion-2 seen in transition zone. 2.3 cms and shows low intensity signal in T2 and ADC images and high signal in DW1 images ( score 5). Seminal vesicle is involved shows low intesnsity signal in T2 and ADC images and high signal in DW1 images. Enhances following contrast media.Left side-lesion 3 seen in peripheral zone mid gland. It measures 0.8 cms in size shows low intensity signal in T2 and ADC images and high signal in DW1 images (score 5). Enhances following contrast media. Lesion 4-seen in transition zone. 1.1 cms and shows low intensity signal in T2 and ADC images and high signal in DW1 images (score 5). Enhances following contrast media.Seminal vesicle is involved shows low intesnsity signal in T2 and ADC images and high signal in DW1 images. Enhances following contrast media. Enalrged lymph node 1.7*1.3 cm seen right periprostatic fat. shows low intensity signal in T1 and T2 images.
Prostate biopsy- Right base (gleason score 8, 30% of total tumor volume) middle (gleason score 9, 50% of total tumor volume) , apex (gleason score 9, 70% of total tumor volume), periphery (gleason score 8, 10-15% of total tumor volume), nodule lobe (gleason score 8, 30% of total tumor volume) – Adenocarcinoma.Left mid (Gleason score 8, 10-15% of total tumor volume)- Adenocarcinoma. Left base and apex- negative for malignancy.
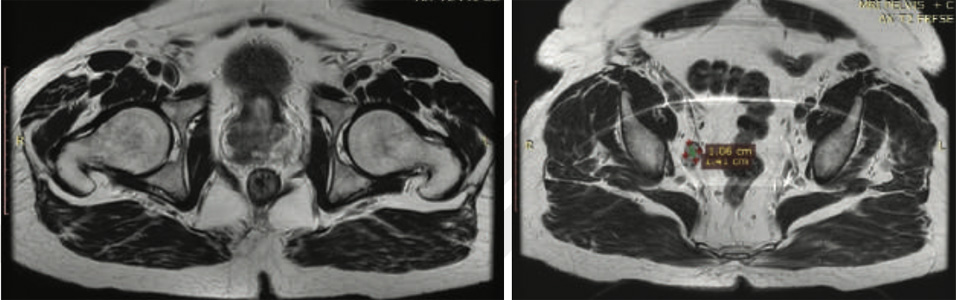
Figure 1- MRI of Prostate
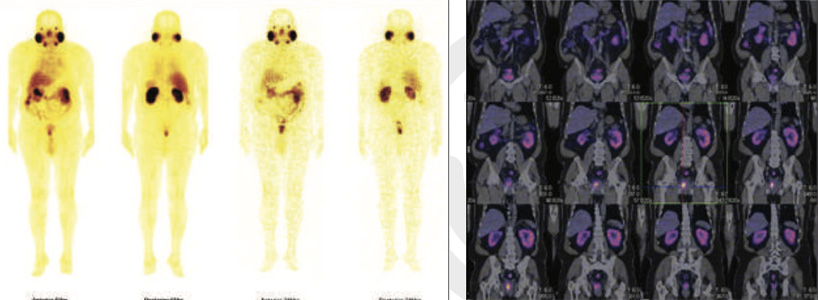
Figure 2 & 3: 99mTc-PSMA whole body images & SPECT CT whole body fused images
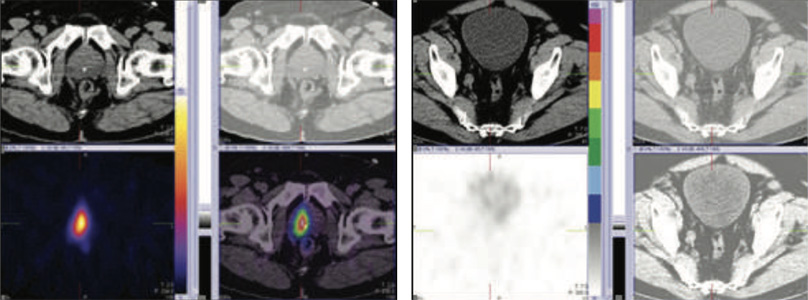
Figure 4 & 5: 99mTc-PSMA SPECT CT fused images of the pelvis
Large sized psma expression lesion seen in right prostatic bed at 5 & 24 hours images.No PSMA expression lesions are seen elsewhere on whole whole body SPECT-CT fused images.
Subsequently patient underwent robotic surgery for prostate removal.
Four months post operatiely- PSA 0.003, So lymph node as mentioned on MRI and not seen on PSMA images looks to be benign at this stage.
Large sized psma expression lesion seen in right prostatic bed at 5 & 24 hours images.No PSMA expression lesions are seen elsewhere on whole whole body SPECT-CT fused images.
Subsequently patient underwent robotic surgery for prostate removal.
Four months post operatiely- PSA 0.003, So lymph node as mentioned on MRI and not seen on PSMA images looks to be benign at this stage.
Ref for 99mTc PSMA SPECT-CT SCAN
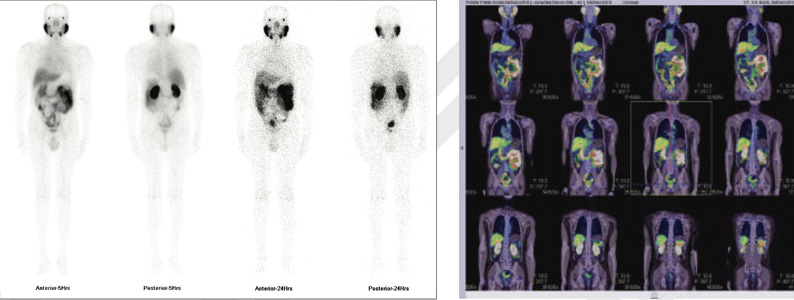
Figure 1 & 2: 99mTc-PSMA whole body images & whole body SPECT CT fused images
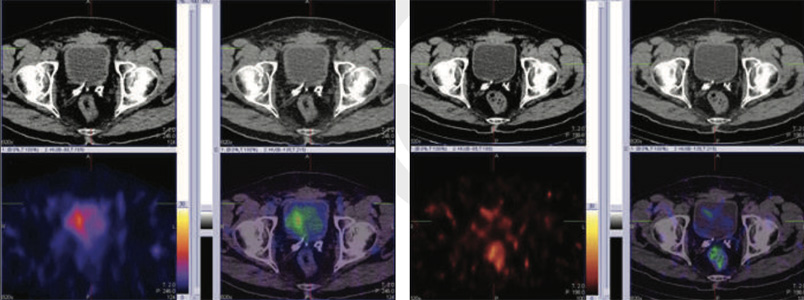
Figure 3 & 4: 99mTc-PSMA SPECT CT fused images of pelvis
No psma expression lesions are seen in prostatic bed nor elsewhere on whole body images.
58 yrs old gentleman with h/o Old prostate biopsy (2012) negative for malignancy.
Dec 2018- went for follow up PSA levels 6.33ng/ml (<4.0) MRI prostate- Enlarged prostate gland with indentation
on the bladder base region. Altered signal intensity of the peripheral region in the proximal portion of the gland,
which is predominantly on the left side of the midline and to lesser extent on right side. There is involvement of
the prostate capsule and left seminal vesicle. Enlarged node is also noted in left internal iliac group.
In view of raised PSA, this region may be associated with neoplastic changes ( PI RADS 4). However post biopsy scarring can not be excluded.
Ref for 99mTc PSMA SPECT-CT SCAN before biopsy.
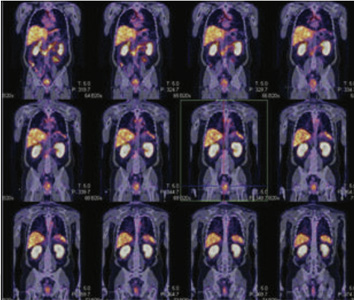
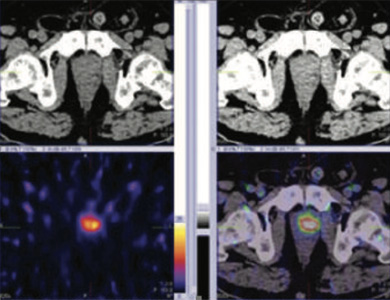
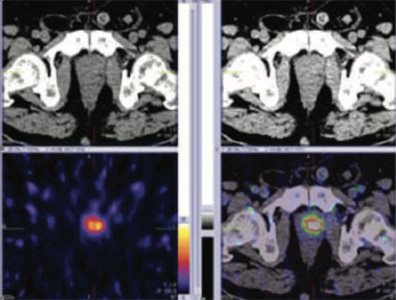
Figure 1 & 2: 99mTc-PSMA whole body SPECT CT fused images & SPECT CT fused images of pelvis
Figure 3: 99mTc-PSMA whole body SPECT CT fused images & SPECT CT fused images of pelvis
PSMA expression lesion seen in base of the prostate in mid line and apex of the prostate. Turp defect PSMA accumulation is true lesion (not urine collection) Rest of whole body images were unremarkable.
Subsequent Prostate biopsy- shows Acinar Adenocarcinoma of prostate
Right base (gleason score 8, 30% of total tumor volume).Right mid 1/3rd (gleason score 8), Right apex (gleason score 8, 31% of total tumor volume), Left base (gleason score 8, 50% of total tumor volume), Left core biopsy (gleason score 8, 71% of total tumor volume).Left Apex (gleason score 8, 85% of total tumor volume).No extra prostatic spread noted.
71 yrs old gentleman, known case of malignant prostate cancer diagnosed in 2017 submitted to radiotherapy followed by total androgen castration in sept 2018.
Following NCCN guidelines, the PSA started to increase in progressive time despite lower normal range but considered to be significant.
27.8.19 8.6.19
PSA levels 0.56 ng/ml 0.34 (<4.0)
Free PSA 0.08 ng/ml 0.05
Ref for 99mTc PSMA SPECT-CT SCAN in view of high PSA values
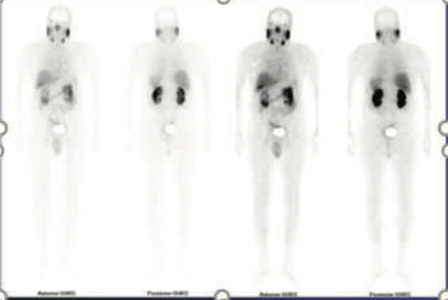
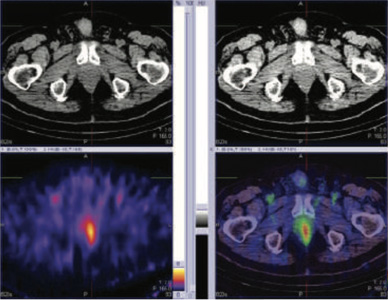
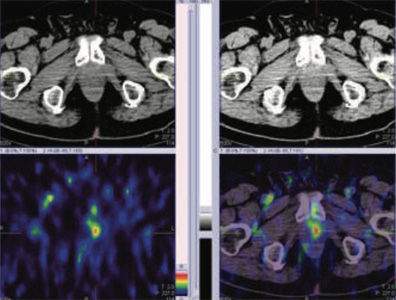
Figure 1: 99mTc-PSMA whole body images
Figure 2 & 3: 99mTc-PSMA SPECT CT fused images of the pelvis
PSMA expression lesion seen in apex of the prostate (left side).
Subsequent Prostate biopsy- shows Adenocarcinoma of prostate
64 yrs old gentleman, known case of BPH & elevated PSA.
His PSA 21.3 ng/ml, inspite of giving him all the medications and alfa blockers. His PSA went up to 27.8 in 6 months.
He had previous biopsy which was negative.
Right base – fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified. Right mid 1/3rd - fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified. Right apex - fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified. Left base- fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified.Left mid 1/3rd biopsy- fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified. Left Apex -fibromuscular tissue with unremarkable rectal mucosa. No glandular tissue identified.
Ref for 99mTc PSMA SPECT-CT SCAN in view of high PSA values
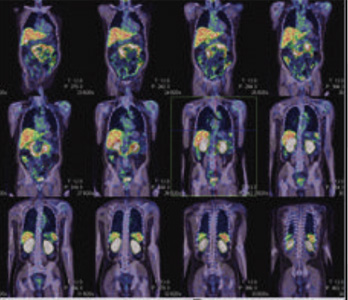
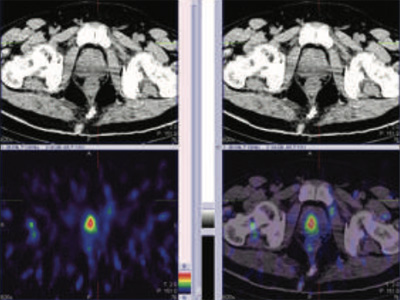
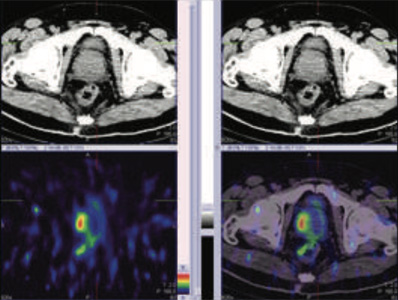
Figure 1 & 2: 99mTc-PSMA whole body SPECT CT fused images & SPECT CT fused images of the pelvis
Figure 3: 99mTc-PSMA SPECT CT fused images of the pelvis
PSMA expression lesion seen in right base & apex of the prostate (mid portion), rest of the whole body images were unremarkable.
Prostate biopsy- Acinar adenocarcinoma of prostate.
56 yrs old gentleman with elevated PSA. PSA 7.56 ng/ml.
Ref for 99mTc PSMA SPECT-CT SCAN in view of high PSA values
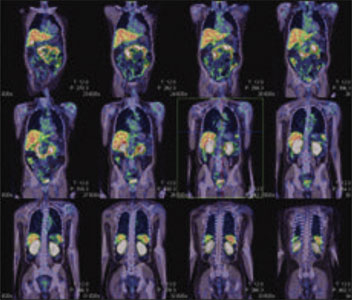
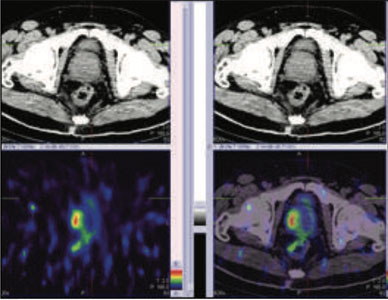
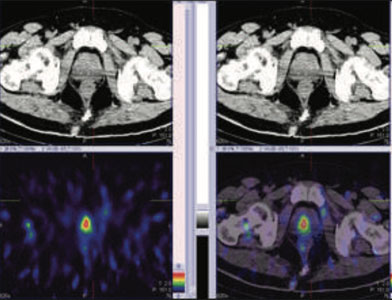
Figure 1: 99mTc-PSMA whole body SPECT CT fused images, Figure 2 &3 : 99mTc-PSMA SPECT CT fused images of the pelvis
PSMA expression lesions are seen in right peripheral zone and mid zone of the prostate. Rest of the whole body images were unremarkable.
Prostate biopsy- Adenocarcinoma of prostate.
66 years old gentleman with symptoms of BPH.
Elevated PSA (Total PSA 11.55 ng/ml) & free PSA 1.010 ng/ml.
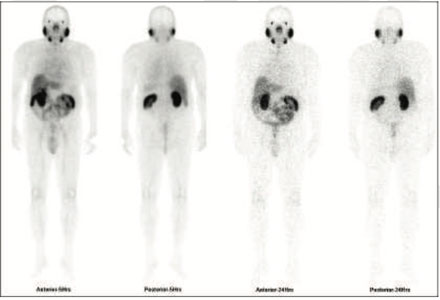
Figure 1: 99mTc-PSMA whole body images
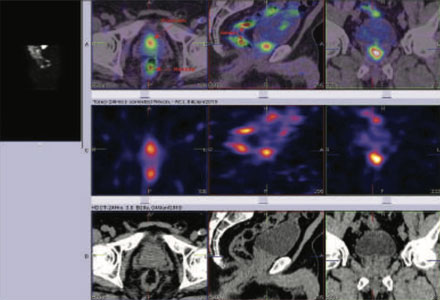
Figure 2 99mTc-PSMA SPECT fused images pelvis
99mTc-PSMA SPECT CT fused images of the pelvis
PSMA expression lesion seen in mid portion of the prostatatic bed.
Rest of the whole body images were unremarkable.
Prostate biopsy- Adenocarcinoma of prostate.
73 years old gentleman with history of increasing lower urinary tract symptoms mainly in the form of frequency and urgency. H/o of DM,HTN and cardiomyopathy. Elevated PSA (Total PSA 30.131 ng/ml)
Ref for 99mTc PSMA SPECT CT SCAN
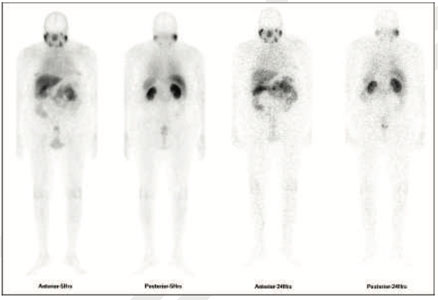
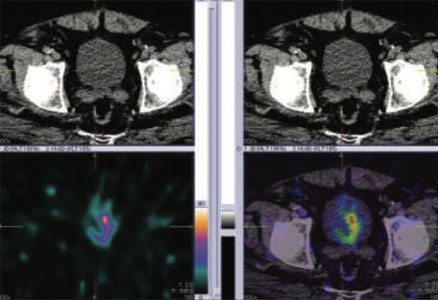
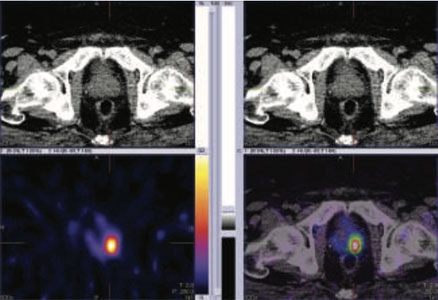
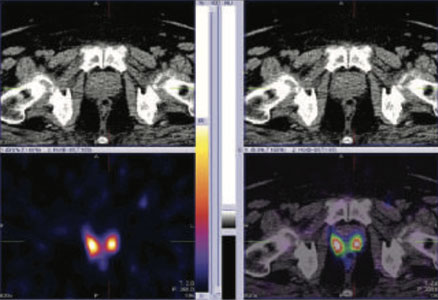
Figure 1: 99mTc-PSMA whole body images, Figure 2,3 & 4: 99mTc-PSMA SPECT fused images pelvis
99mTc-PSMA SPECT CT fused images of the pelvis
PSMA expression lesion seen involving most of the prostatatic bed.
Rest of the whole body images were unremarkable.
Prostate Biopsy- Adenocarcinoma of prostate.
A. Prsotate right base core biospy- Adenocarcinoma of usual type involving two cores. Gleason score 4+5=9 & 3+4=7 involving 80% & 100% of the cores. The tumour measuring 7 mm & 6 mm respectively. Patterns 5 involves 15% of the tumour and pattern 4 involves 25% of the tomour. No perineural or extra prostatic extension identified.
B. Prostate gland 1/3rd of medial right core biopsy- Adenocarcinoma of usual type involving all four cores. Gleason score 3+4=7 involving 100%, 80%, 90% & 80% respectively, measuring 5 mm ,6 mm, 5 mm & 6 mm respectively. Patterns 4 involves 25%, 20%,10% & 5% of the tumour. of the tumour. No perineural or extra prostatic extension identified.
C. Prostate apex right core biospy- Adenocarcinoma of usual type involving all three cores. Gleason score 4+4=8, 4+3=7, 3+3=6 involving 20%, 70% & 50% of the cores , measuring 3 mm ,5 mm & 6 mm respectively. Patterns 4 involves 40% of the tumour in two cores. of the tumour. Perineural invasion is present. No extra prostatic extension identified.
D. Prostae base left core biopsy- Adenocarcinoma of usual type, Gleason score 4+4=8 involving all three cores 30%, 80% & 40% of the cores , measuring 4 mm discontinuous,10 mm & 3 mm respectively. Patterns 4 involves 40% of the tumour in two cores. of the tumour. Perineural invasion is present. No extra prostatic extension identified.
E. Prostae 1/3rd medial left core biopsy- Adenocarcinoma of usual type involving all 3 cores, Gleason score 4+3=7 involving 90%, 40% & 40% , measuring 9 mm,2 mm & 3 mm respectively. Patterns 4 involves 100% & 50% of the tumour. No perineural or extra prostatic extension identified.
F. Prostae apex left core biopsy- Adenocarcinoma of usual type, Gleason score 4+5=9 involving one of the two cores 50% of the core, measuring 4 mm. Patterns 5 involves 20% of the tumour.in No perineural or extra prostatic extension identified.
71 years old gentleman, known case of prostate cancer diagnosed 2017 submitted to radiotherapy followed by total androgen castration concluded in September 2018 and reached undetectable PSA. The PSA serum levels started to increase in progressive time, despite in lower range but considered significant for further therapeutic treatment (PSA levels 0.120 ng/ml).
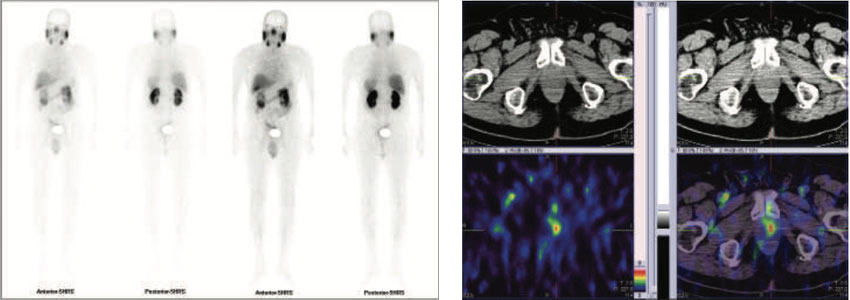
Figure 1 & 2 : 99mTc-PSMA whole body images & SPECT CT fused images of the pelvis
PSMA expression lesion seen in apex of the prostate (left side). Rest of the whole body images are unremarkable.
73 years old gentleman with history of increase in frequency of urination. KUB- Prostate enlargement with evidence of bladder outlet obstruction. Bilateral non obstructive nephrolithiases, multiple in left kidney PSA levels 93.06 ng/ml
A. Prsotate right base core biospy- Adenocarcinoma gleason grade group 4 (Gleason scroe 4+4=8 ) involving 90% &50% of the cores. No perineural or extra prostatic extension identified.
B. Prostate gland middle right core biopsy- Adenocarcinoma gleason grade group 4. Gleason score 4+4=8 involving 50%, 50% & 80% of the three cores. Perineural invasion is present. No extra prostatic extension identified.
C. Prostate apex right core biospy- Adenocarcinoma gleason grade group 4. Gleason score 4+4=8) 4+3=7, 3+3=6 involving 70% & 60% of the cores. Perineural invasion is present. No extra prostatic extension identified.
D. Prostae base left core biopsy- Adenocarcinoma gleason grade group 4. Gleason score 4+4=8 ) involving 60% of the core. No perineural invasion is present. No extra prostatic extension identified.
E. Prostae middle left core biopsy- Adenocarcinoma gleason grade group 4. Gleason scroe 4+4=8) involving 30% &60% of the core. No perineural invasion is present. No extra prostatic extension identified.
E. Prostae middle left core biopsy- Adenocarcinoma gleason grade group 4. Gleason scroe 4+4=8) involving 30% & 60% of the 2 cores respectively. No perineural or extra prostatic extension identified.
F. Prostae apex left core biopsy- Adenocarcinoma gleason grade group 4 (Gleason scroe 4+4=8) involving 30% of the core. Perineural invasion is present. No evidence of extra prostatic extension seen.
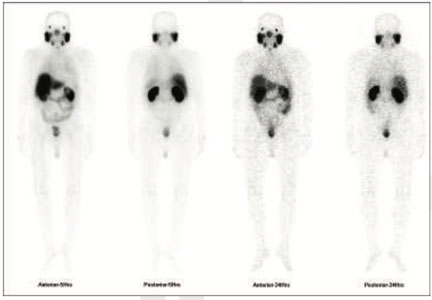
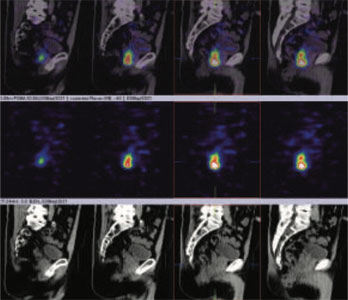
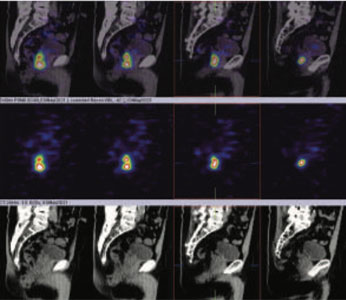
Figure 1: 99mTc-PSMA whole body images
figure 2 & 3 (sagittal view): 99mTc-PSMA hybrid SPECT CT fused images of the pelvis
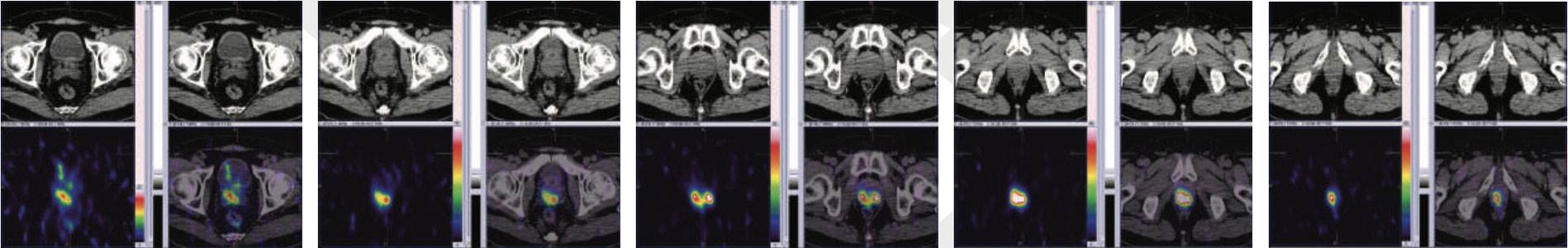
figure 4 to 8 (axial view): 99mTc-PSMA hybrid SPECT CT fused images of the pelvis
PSMA expression lesion seen involving whole of the prostate gland from base to apex and extending from center towards periphery (figure 2 to 8).Rest of the whole-body images are unremarkable (figure 1)
70 years old gentleman referred for 99mTc PSMA HYBRID spect ct scan for the staging of the disease process.
PSA levels 21 ng/ml
Prostate Biopsy- Adenocarcinoma of prostate.
With Gleason score=4+5=9 in all cores. The degree of involment of the cores is between 40 to 60%
Whole body images are obtained at 5 Hrs, 24 Hrs and whole-body Hybrid SPECT- CT Fused Images at 24 Hrs.
Prostate
It shows abnormal avid PSMA tracer accumulation seen involving whole of the prostate gland (Base to apex). Left side is more than the right side.
Abnormal avid PSMA tracer uptakes seen in
a) Most of the lymph nodes in pelvis adjacent to prostate gland (obturator, internal iliac). Right side is more than the left side.
b) Common iliac and aorto-caval lymph nodes on right side.
Right side - Subcarinal and hilar lymph nodes and axillary lymph nodes.
Left side- Subcarinal, hilar lymph node & para-aortic lymph node.
NOTE- Tracer uptake pattern is asymmetrical in nature and more so avid on the right side.
Small area of abnormal PSMA tracer uptakes seen D11/D12 vertebra (linear in shape on sagittal view with no underlying CT scan abnormality except osteophytes)
Rest Of The Whole Body And hybrid SPECT-CT Images shows No obvious abnormal PSMA tracer uptakes.
Normal tracer uptake visualization in Salivary glands supra orbitor region laterally, liver, kidneys, intestine, and bladder etc.
PSMA AVID LESIONS ARE SEEN IN PROSTATE GLAND, PELVIC, ABDOMINAL AND CHEST LYMPH NODES AS DESCRIBED ABOVE, LIKELY TO REPRESENTS PROSTATE CANCER WITH LYMPH NODE METASTASIS
REST OF THE WHOLE-BODY IMAGES ARE UNREMARKABLE.
Note- The subcarinal, hilar lymph node and axillary lymph node involvement commonly seen with active granulomatous disease (sarcoidosis) and shows bilateral symmetrical involvement of the lymph nodes.
In this case there is asymmetrical avid lymph node tracer uptake is seen (right side>left side) and hence likely to metastatic as first choice though its not common site.
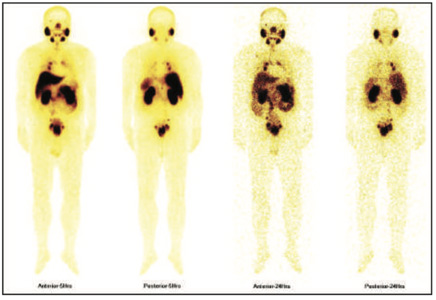
99mTc PSMA whole body scan at 5 hours and 24 hours
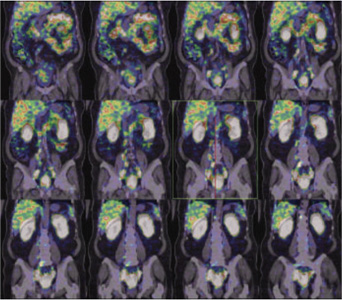
99mTc PSMA hybrid SPECT CT images of the pelvis and abdomen at 24 hours
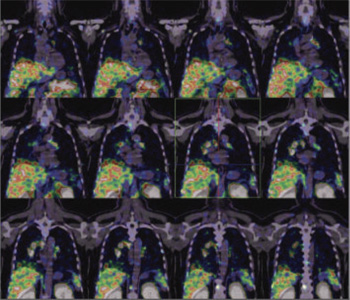
99mTc PSMA hybrid SPECT CT images of the chest at 24 hours

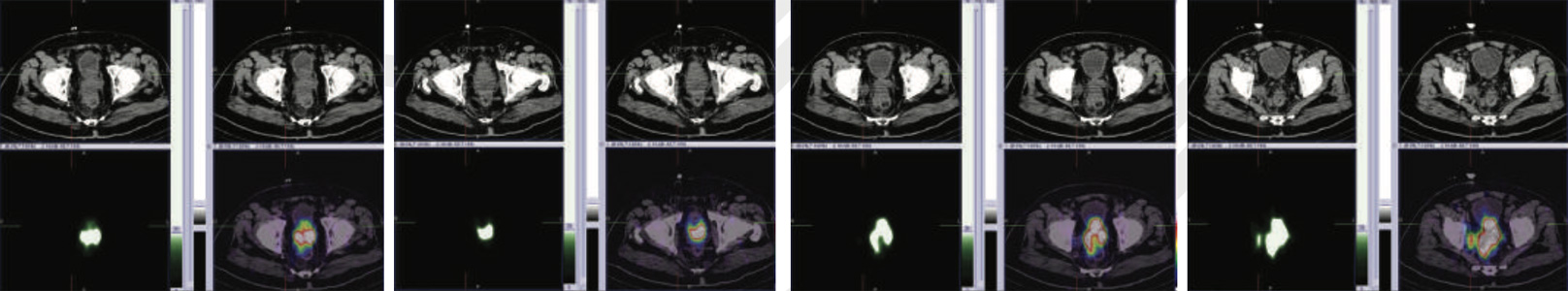
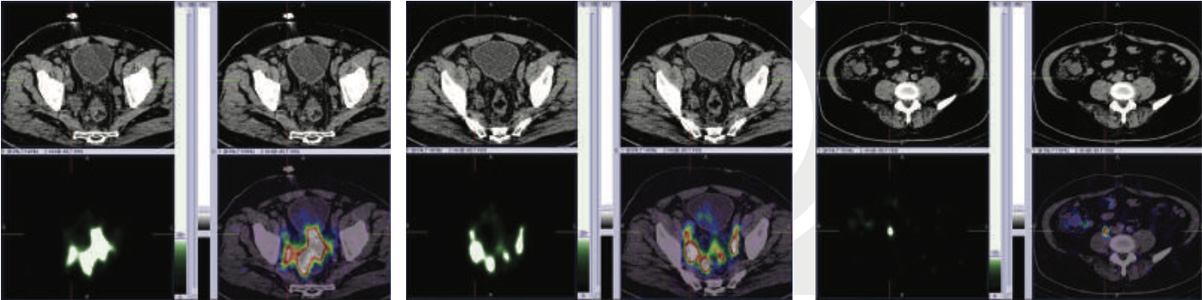
99mTc PSMA hybrid SPECT CT images of the pelvis and abdomen at 24 hours
66 years old gentleman referred for 99mTc PSMA HYBRID SPECT CT scan for the staging of the disease process.
MRI SCAN OF THE PELVIS WITH AND WITHOUT CONTRAST A diffuse enlargement of the prostate gland with its central/transitional zone. As compared to old MRI shows increase in size, heterogeneous signal and suggestion of diffuse restriction in the corresponding sequence. This along with raised PSA levels may suggest development of neoplastic changes on the underlying hypertrophic psostate ( PI-RADS 4). The prostate enlargement appears to be confined ( intact prostatic capsule) with no obvious local extension evident. Rest of the pelvis study appears to be normal.
Prostate base right negative for malignancy.
Prostate 1/3rd medial right -prostatic acinar adenocarcinoma, Gleason score 3+3=6/10. Tumor invloves once core and nearly 25% of the tissue. No evidence of perineural or lymphovascular invasion.
Prostate apex right prostatic acinar adenocarcinoma, gleason score 3+3=6/10. Tumor involves one core and nearly 20% of the tissue.No evidence of perineural or lymphovascular invasion.
Prostae base left- no evicence of mailgnncy.
Prostate 1/3rd medial negative for malignancy.
Prostate apex left negative for malignancy.
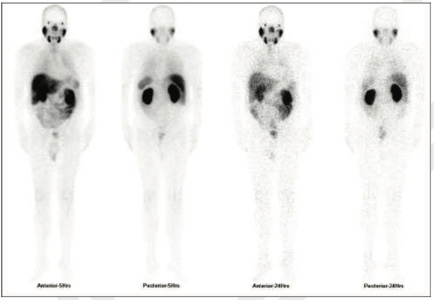
99mTc PSMA whole body scan at 5 hours and 24 hours
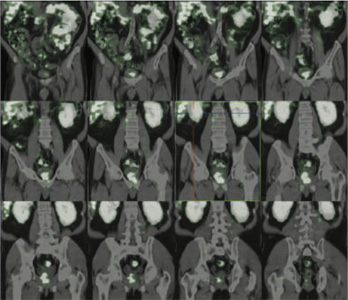
99mTc PSMA hybrid SPECT CT images of the pelvis and abdomen at 24 hours
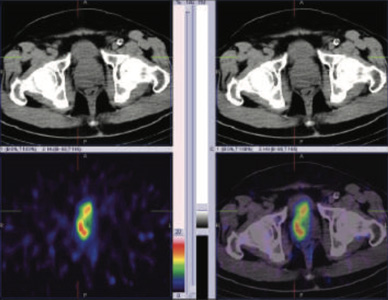
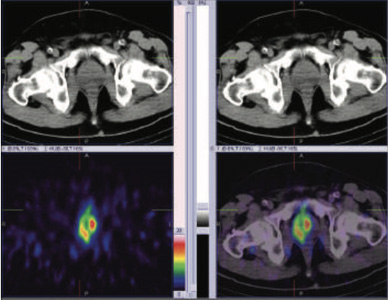
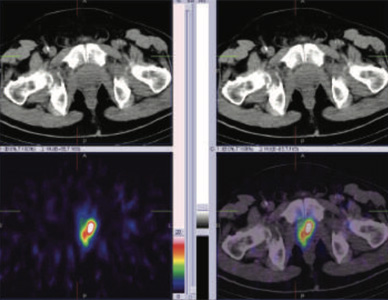
99mTc PSMA hybrid SPECT CT images of the pelvis at 24 hours
60 years old gentleman referred for 99mTc PSMA HYBRID SPECT CT scan for the staging of the disease process.
PSA levels 11.710 ng/ml ( 0-4).
Prostate base right negative for malignancy.
Prostate 1/3rd medial right - negative for malignancy
Prostate apex right negative for malignancy.
Prostae base left core biopsy- Prostate acinar adenocarcinoma gleason score 3+4=7 Tumor involves both cores and nearly 70% of tisue. No perineural invasion is present. No extra prostatic extension identified.
Prostae middle left core biopsy- Prostate acinar adenocarcinoma gleason score 3+4=7 Tumor involves all three cores and nearly 40% of tisue. No perineural invasion is present. No extra prostatic extension identified.
Prostae apex left core biopsy- Prostate acinar adenocarcinoma gleason score 3+4=7 Tumor involvves both cores and nearly 70% of tisue. No perineural invasion is present. No extra prostatic extension identified.
Acinar adenocarcinoma of prostate ( left side) . With Gleason score=3+4=7
99mTc- LABELLED-PSMA ( 584.6 MBq) WHOLE BODY SCAN {PSMA-PROSTATE SPECIFIC MEMBRANE ANTIGEN)
Whole body images are obtained at 5 Hrs, 24 Hrs and Spect- CT Fused Images of
a) Whole body 5 Hrs
b) Pelvis at 24 Hrs
Focal area of abnormal PSMA tracer accumulation seen in prostatic gland left side and appreciated at 24 hours HYBRID images.
Rest Of The Whole Body And SPECT-CT Fused Images shows No obvious abnormal PSMA tracer Uptakes in Skeletal, Liver, Lung And Lymph Nodes etc.
Normal tracer uptake visualization in Salivary glands supra orbitor region laterally, liver, kidneys, intestine and bladder etc.
Comments
The Study Suggests:
PSMA Avid Tissue Abnormality Seen In Prostate Gland (Left Side) And Apprecited At 24 Hours Spect Ct Fussed Images).
Rest of the whole-body images are unremarkable.
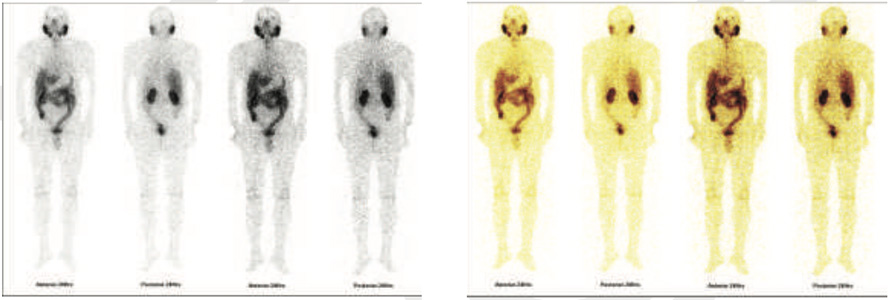
99mTc PSMA whole body scan at 24 hours
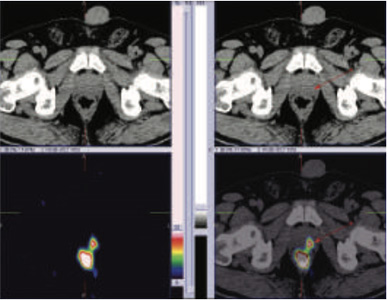
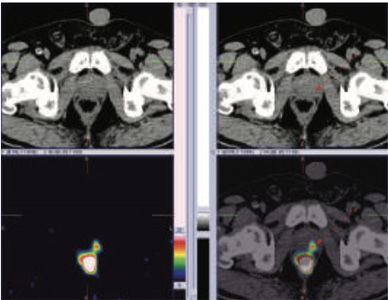
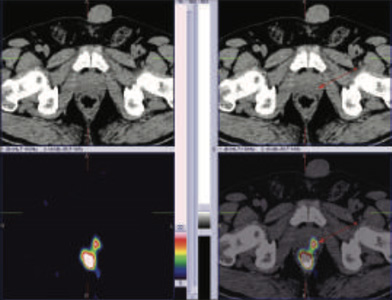
99mTc PSMA hybrid SPECT CT images of the pelvis at 24 hours
60 years old gentleman referred for 99mTc PSMA HYBRID SPECT CT scan for the staging of the disease process.
67 years old gentleman is a Known case of adenocarcinoma underwent radicle prostatectomy two years ago and on casodex & zoladex, now slightly elevated PSA and pain in left hip laterally.
referred for 99mTc PSMA HYBRID SPECT CT scan for the staging of the disease process.
PSA levels ( 0-4). 21.8.21 13.11.21 7.2.22
0.010 ng/ml 0.020 ng/ml 0.020 ng/ml
Whole body images are obtained at 5 Hrs, 24 Hrs and Spect- CT Fused Images of
a) WHOLE BODY 5 Hours
b) Pelvis at 24 Hrs
No obvious focal area of abnormal PSMA tracer accumulation seen in prostatic bed on hybrid whole body images.
Rest Of The Whole Body And Hybrid SPECT-CT Images shows No obvious abnormal PSMA tracer Uptakes in Skeletal, Liver, Lung And Lymph Nodes etc.
Normal tracer uptake visualization in Salivary glands supra orbitor region laterally, liver, kidneys, intestine and bladder etc.
COMMENTS:The Study suggests
No Obvious Abnormal PSMA Avid Tissue as well as Skeletal Abnormality is seen on present study.
Rest of the whole-body images are also unremarkable.
Underlying CT images of pelvis (as per radiologist) shows bilateral trochanteric bursitis (left>right).
X Ray pelvis- Osteophytesa are seen from the margins of the acetabulum and dystrophic calcification noted at the greator trochnaters possible associated with the gluteal tendon insertions.
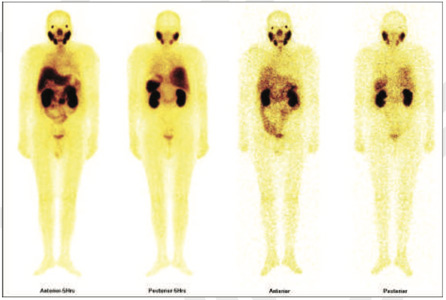
99mTc PSMA whole body scan at 5 hours
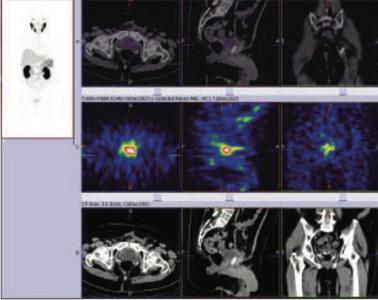
99mTc PSMA hybrid SPECT CT images of the pelvis at 5 hours
Molecular imaging used for prostate cancer? By the physician to:
Stage: by determining the exact location of a tumor, the extent or stage of the disease and whether the cancer
has spread in the body. Plan treatment: by selecting the most effective therapy based on the unique molecular
properties of the disease and of the patient’s genetic makeup
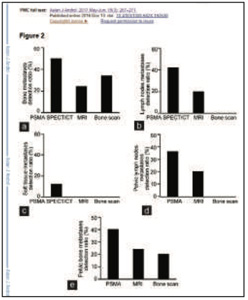
The diagnostic efficiency of PSMA-SPECT/CT Imaging for different metastatic lesions in PCa patients. The efficiency of PSMA-SPECT/CT imaging in a) diagnosing bone, (b) lymph node, and (c) soft-tissue metastases was greater than bone scan or MRI .The diagnostic efficiency on (d) pelvic lymph node metastases and pelvic bone metastases with PSMA SPECT/CT imaging was better than bone scan and MRI
Asian Journal of andrology, year 2017, vol19, issue3
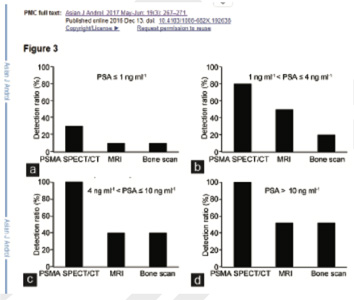
PSMA-SPECT/CT provided a higher detection rate at 1–4 ng ml−1 ..
Asian Journal of andrology, year 2017, vol19, issue3
PMSA studies are able to determine the extent of prostate cancer and whether it has spread to the lymph nodes or other parts of the body, unlike traditional imaging technologies such as magnetic resonance imaging (MRI) and computed tomography (CT), which are often unable to detect the spread of prostate cancer cells.
Evaluation of 99mTc-labeled PSMA-SPECT/CT imaging in prostate cancer patients who have undergone biochemical relapse.
Heng-Chuan Su,1,2,* Yao Zhu,1,2,* Guo-Wen Ling,1,2 Si-Long Hu,3 Xiao-Ping Xu,3 Bo Dai,1,2 and Ding-Wei Ye1,2 Asian J Androl. 2017 May-Jun; 19(3): 267–271.
Direct comparison of 99mTc-PSMA SPECT/CT and 68Ga-PSMA PET/CT in patients with prostate cancer. Batool Albalooshi,1 Mouza Al sharhan,2 Fariborz Bagheri,3 Shabna Miyanath,1 Bhavna Ray,1 Muhammed Muhasin,1 and Seyed Rasoul Zakavi. Asia Ocean J Nucl Med Biol. 2020 Winter; 8(1): 1–7.
99mTc-PSMA SPECT/CT verses 68Ga-PSMA PET/CT in the evaluation of metasatic prostate cancer. Babak Fallahi 1, Niloufar Khademi 1, Najme Karamzade-Ziarati 1, Armaghan Fard-Esfahani 1, Alireza Emami-Ardekani 1, Saeed Farzanefar 2, Mohammad Eftekhari 1, Davood Beiki Clin Nucl Med 2021 Feb 1;46(2):e68-e74.1