Skull base osteomyelitis (SBO) is an infection of the temporal, sphenoid, or occipital bones that is typically caused by a complication of Sino nasal infection in elderly patients with diabetes or immunocompromised patient.
SBO is a rare life-threatening disease with nonspecific symptoms. Several diseases can mimic SBO at imaging, and SBO can be misinterpreted as a malignancy. The diagnosis of SBO is therefore often delayed, and a high index of clinical suspicion is required.
The skull base has a complex anatomy formed by the frontal, temporal, occipital, ethmoid, and sphenoid bones. From an endocranial view, the skull base can be subdivided into three regions: anterior, central, and posterior. The anterior to central skull base regions are separated by the posterior margin of the lesser wing of the sphenoid bone, the anterior clinoid processes, the tuberculum sellae, and the anterior margin of the greater wing of the sphenoid bone. The border between the central and posterior skull base regions is the superior margin of the petrous part of the temporal bone and the dorsum sellae.
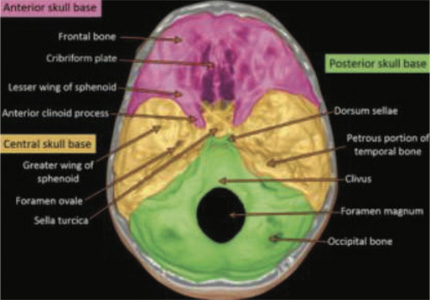
The anatomy of the central skull base is complicated owing to the confluence of numerous essential structures. This region contains cavernous sinuses that are crossed by both internal carotid arteries and the oculomotor (III), trochlear (IV), ophthalmic, and maxillary divisions of the trigeminal (V1 and V2) and abducens (VI) nerves. The cranial nerve V2 leaves the cavernous sinus, traveling toward the foramen rotundum and arriving at the pterygopalatine fossa. Another important structure is the orbital apex with the optic canal, which is crossed by the optic nerve (II) and the superior orbital fissure, which provides a passage for cranial nerves III, IV, VI, and V1.

56 years old gentleman admitted with fever, cough, dysnea & reduced oxygen satuaration since last seven days with positive Covid-19 PCR tests few weeks ago. Treated with high flow nasal oxygen, injection tocilizumab, favipiravir, intravenous steroids, anticoagnulation and supportive care. Patient gradually improved clinically and weaned off oxygen supplement and discharged.
Post discharge continues to be on steroids, supportive medications for next few weeks and anti diabetic medications for his uncontolled diabetes mellitus.
Lateky started complaining of severe headache, recurrent rhinitis, left hearing loss.
MRI BRAIN- shows age apprpriate cerebral atrophy with multiple small areas of T2 falir hyperintensity bilateral periventricular and subcortcial white matter fronto parietal region? small vessel ischemic disease.
Petrous temporal bones- partial obliteration of the mastoid air cells bilaterally, in keeping with chrnoic mastoiditis. Obliteration of the left middle ear cavity with mild mucosal thickening of the right middle ear cavity, in keeping with bilateral chronic ostitis media (more on left side).
Evidece of significant rarefication, demineralisation and erosions of the bones of the skull base, mainly involving clivus as well as surrounding parts of the sphenoid bone as well as maxilla particularly along with posterior inferior aspect of maxillary sinuses and alveolar margins more on the left side- Suggestive of skull base osteomyelitis particularly considering the associated findings of chronic rhinosinusitis and otomastoididitis.
Follow up CT scan of paranasal sinuses (non contrast) after four weeks shows
There is diffuse circumferential mucosal thickening with soft tissue opacification noted in paranasal predominantly filling the right frontal, bilateral sphenoid sinus associated with non visulaisation of right middle turbinate and nasal septum likley suggesting invasive fungal sinusitis. The sapenous mass opacification eroding destructive posterior wall sphenoid sinuses extended infiltrated posteriooryl invading the attenuated rarefied destructive clivus basal skull with eroding ints cortcial outline, the bony erosion extended into thickned bilateral frontal bones eroding anterior/posterior tables right frontal bone including right orbitor roof and erosding anterior tables left frontal bone likely to represented with osteomyelitis infiltration. Attenuated with rareficationand bony erosion including the expandedbilateral lateral walls and basal maxillary bones. No flid collection is seen. Obliteration of right osteomeatal complex unit Finding likley representing with diffuse invasive fungal sinusitis associated with destructive bony erosion likley of osteomyelitis sequuelae.
Patient subsequntley underwent
a) Opening of all the sinuses, which shows sigfificant mucosal inflammation, fungal growth along with necrotic tissue, which has been removed. Microsopic examination showed aspergillus growth with psedomonas.
b) Bilateral myringotomy and bilateral grommet insertion was done. It shows clear fluid.
c) On antifungal medications, antibiotics and anti diabetic medictauions (Diabetes is well controlled)
Diagnosis- Central skull base osteomyelitis with invasive fungal sinusitis (aspergillus growth with psedomonas)
Follow up CT scan of paranasal sinuses four weeks postoeratively
Expansion of frontal bone with hyperostosis thickening sclerosis of the permeative eroded/destructive anterior/posterior table out linefrontal bone involving ethmoid plate with internal bony sensity opacification within doplioc space and anterior soft tissue thickening more on the right side but no sign on intracranial brain involvment likley representing with findings of the osteomyelitis sequelae. Lytic permeative bony destruction of the clivus bone with sella turcica and psoterior sphenoidal wall involvement. Diffuse mucosal swelling thikening soft tissue opacification of bilateral paranasal sinuses with eroded nasal septum and non visualised middle turbinates . No flis collection is seen. Non visualised bilateral medal wall of maxillary sinuses.
Findings likely representing with diffuse opacification of paranasal sinuses associated with bony destruction of clivus and frontal none likley of ostemyelitis sequelae.
Referred for Isotope bone scan for better characterisation of osteomyeltis sequelae, extent and severity of the diease process and to rule out acute from chronic osteomyelitis.
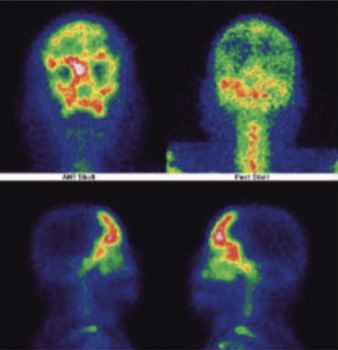
99mTc MDP whole body bone & hybrid SPECT CT images of the skull ( three phase bone scan)
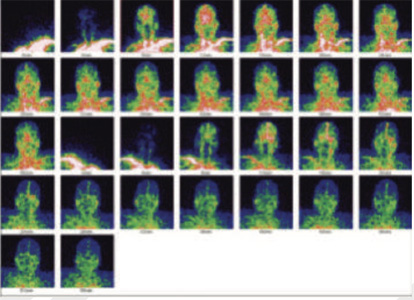
Blood flow images of the skull
99mTc-MDP blood flow images of the skull shows increased perfusion bifrontally and adjoing areas.
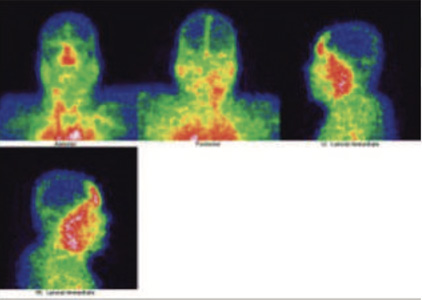
99 m Tc MDP Satic blood pool images of the skull
99mTc MDP Hybrid SPECT CT blood pool images of the skull
99mTc- MDP blood images of skull shows abnormal pooling for the tracer bifrntally, which is extending to the ethmoid and sphenoidal regions.
99m Tc- MDP Static bone images of the skull
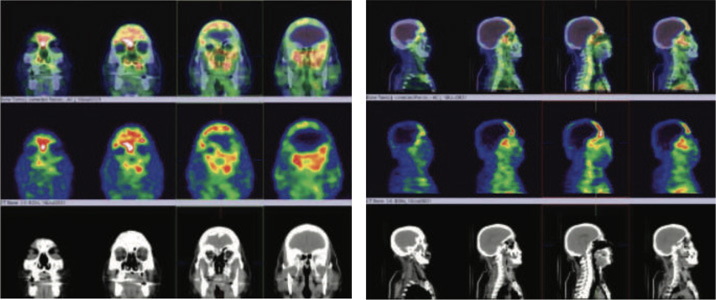
99m Tc- MDP Hybrid SPECT CT bone images of the skull
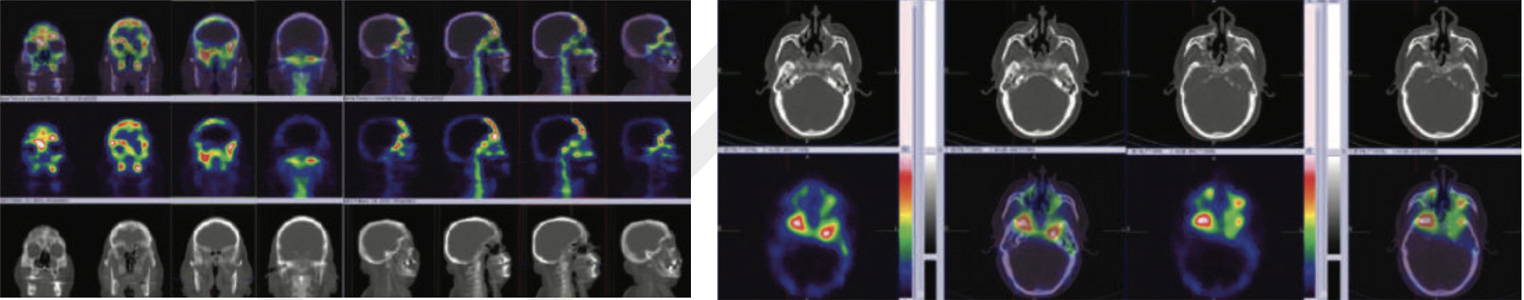
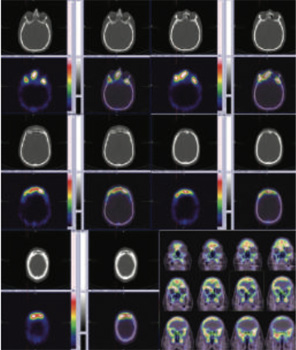
99mTc-MDP Hbrid SPECT CT of skull shows abnormally increased tracer uptake of varying intensities involving central skull base bones- predominantly involving sphenoid bones, which is extending to either sides of mid line with extension to the ethmoid, anterior frontals and maxillary antra.
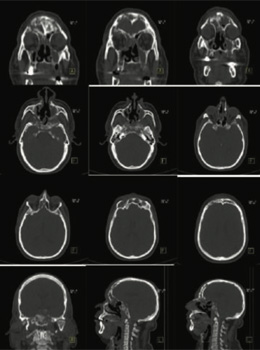
Conclusion- Active extensive osteomyelitis involvingcentral skull base bones- predominantly involving sphenoid bone, which is extending to either sides of mid line with extension to the ethmoid, anterior frontals and maxillary antra (Highly abnormal three phase bone images of the skull).
Underlying CT scan images shows extensive bone involvement affecting the central skull base, predominantly involving the sphenoid bone extending to either side of the midline with extension to the ethmoid and anterior frontals and also extension to both maxillary antra (involving bony walls of the sinuses)
Elderly, diabetic, immunocompromised predominantly male patients are mostly at risk. According to Sreepada et al., in diabetes, there is defective chemotaxis and phagocytosis of polymorphonuclear leukocytes (PMNs), monocytes, and macrophages. The oxidative burst and killing function of PMNs are also shown to be reduced in diabetics predisposing them to infection.
Generally, they present with headache or deep-seated pain, often intractable, as the lone main symptoms (as in this case)
Routine blood investigations generally reveal a normal picture except for the uncontrolled diabetic status and elevated acute phase reactants, especially ESR and CRP. This helps in differentiating between malignancy and skull base osteomyelitis, as it is unlikely to expect elevated acute phase reactants with malignancy. ESR and CRP monitoring is vital as its normalization would indicate the subsidence of infection and thus has an important role in defining the duration of treatment (at present CRP is >45)
A variety of imaging modalities can be used for assessment of these patients and of these MRI is probably the most important. Even though MRI cannot detect bone destruction, the superior soft tissue discrimination is useful for analyzing the soft tissue planes around the skull base and medullary cavity of the bone. The most common MR findings of osteomyelitis include marrow T1 hypo intensity and T2 hyperintensity. Clival enhancement can also be seen, but it poses a diagnostic challenge as it can be seen with neoplast.
CT scan helps to evaluate the extent and severity of SBO by detecting bone erosion, but more than 30 % of affected bone should be demineralized before it is evident and hence, early findings are limited to soft tissue inflammation. The major drawback of CT is that the changes fail to resolve for a long time after treatment is finished, so the use of it as a tool for follow-up is not advised.
So, both MRI and CT scan are complementary to each other and hence, both are advocated to get as much information as possible.
Bone scintigraphy with 99mTc MDP has high sensitivity in diagnosis of patients with SBO. This is attributed to the fact that this radiotracer concentrates in areas with increased osteoblastic activity as found in infection, trauma, and neoplasm. 99mTc MDP bone scan allows earlier diagnosis of osteomyelitis than CT, as it can detect as little as 10% of the bone demineralization. Slow progression of periosteal reaction and bone formation in diabetic patients compared to nondiabetics renders radiographic changes less sensitive in diagnosis of those patients. Hence, combination of radiological and radionuclide imaging is needed for initial diagnosis and follow-up of the treatment response. Hybrid SPECT/CT enables us to achieve a high sensitivity with exact localization, extent and correlation with underlying CT changes.
Technetium-99m methylene diphosphonate (MDP) bone scans, and Hybrid SPECT CT also have an advantage in detecting postoperative osteomyelitis and plays an important role in the follow-up of patients on antibiotics as marrow signal persists for up to 6 months after successful treatment.
Pseudomonas aeruginosa is the most common pathogen implicated in osteomyelitis secondary to malignant otitis externa This seems true for central SBO also, although other organisms have been reported, including Aspergillus. Fungal SBO has been reported to be mostly caused by Aspergillus (as seen in our case)
Although, underlying diabetes and primary or acquired immunodeficiencies have often been evident (in this case uncontrolled diabetes with prolong course of steroids for the Covid 19 treatment).
Patients with fungal SBO were more likely to have underlying chronic sinus disease, symptoms attributable to invasive sinus infection (sin facial pain, periorbital swelling, nasal stuffiness/discharge), but with a relative paucity of features attributable to ear infection. Indeed, the absence of purulent ear discharge was a sensitive (91 %) predictor of underlying fungal SBO.
The management of SBO should be dealt with a multidimensional approach. This approach includes prolonged culture guided antimicrobial therapy with control of underlying comorbid factors such as aggressive glycemic control in diabetes and improvements in immune status in immunocompromised patients. The duration of antimicrobial therapy is variable among the cases reported, but in each case, treatment is to be given for at least 1 month and up to 6 months or more.
The role of surgery is confined to biopsy, drainage of abscess if any, and removal of sequestrate by surgical debridement. This helps in source reduction and decreases inflammatory load while improving the availability of antimicrobial agents to the affected region. The tissue sample plays a vital role in substantiating the diagnosis of SBO by histopathology and microbiology to exclude malignancy.
As expected, amphotericin B is the drug most commonly used in the treatment of Aspergillus osteomyelitis, followed by two azoles: itraconazole and voriconazole.
Central skull base osteomyelitis is a rare, life-threatening condition and that secondary to invasive aspergillosis presenting with severe headache, recurrent rhinitis, left hearing loss in our case.
A systematic analysis of clinical features, imaging, inflammatory markers augmented with histological and microbiological assessment can only help us to reach the correct diagnosis. Early initiation of antibiotic/antifungal therapy is desirable to lower the risk of potential sequelae, which can prove to be fatal. The duration of treatment is guided by clinical findings, normalization of inflammatory markers, and resolution on the bone scan if available.